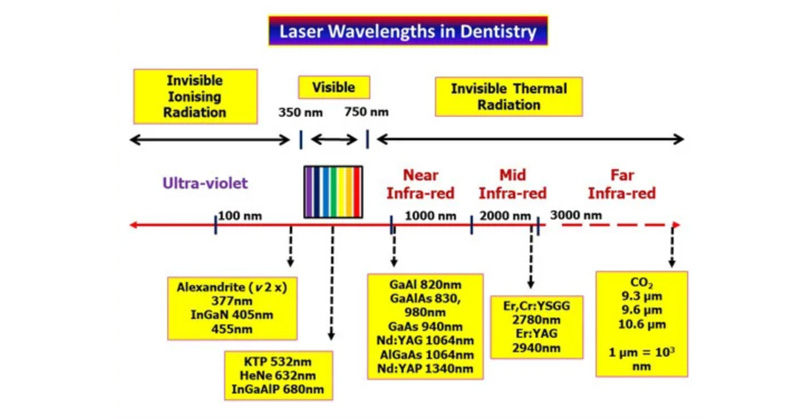
All dental lasers exert their desired clinical effect on a patient’s target tissue by a process called absorption.
1. This target may consist of hard tissue, including natural tooth structure, carious enamel and dentin, dental calculus, bone, or even an existing defective composite restoration within the tooth. Dental lasers function by producing waves of photons (quanta of light) that are specific to each laser wavelength.
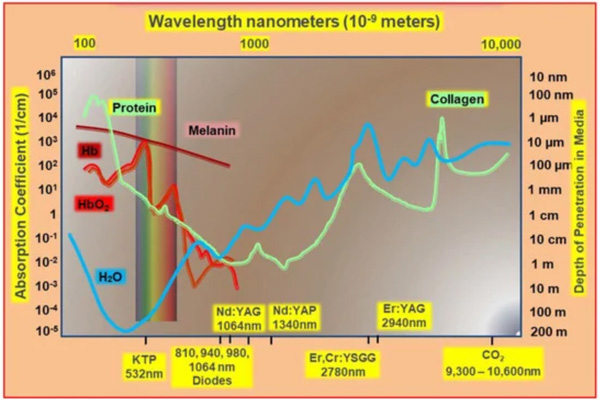
2. This photonic absorption within the target tissue results in an intracellular and/or intercellular change to produce the desired result. It is the basis for a dental laser’s functional dynamic process, referred to as a laser/tissue interaction.
①Nearly all surgical dental lasers function via this wavelength-specific photonic absorption, which causes the temperature within the target tissue cells to increase very rapidly to an evaporative state. These dental lasers cut tissue by a functional process known as a photothermal interaction or photothermal ablation.
②A typical example is the clinical use of a diode, a laser that is utilized in dentistry to treat soft tissue only.3The chromophore of diode lasers is pigmented (or colored) tissues, specifically melanin, hemoglobin (Hb), and oxyhemoglobin.
③The diode is efficient for treating a patient’s soft tissues because gingival tissues have a concentration of these chromophores; as a result, a diode photon has a high affinity for gingival tissues. Diode lasers are used in contact with a patient’s soft tissue to perform common dental procedures such as gingivectomies or soft tissue lesion (fibroma) removal.
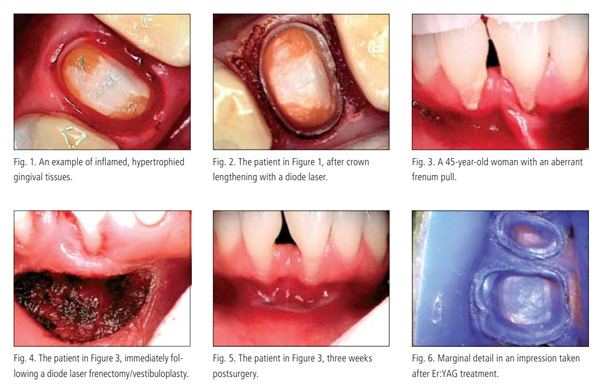
3. Dental lasers offer a number of clinical advantages (especially for soft tissues), including hemostasis (the sealing of local vasculature), the ability to seal nerve endings and lymphatic vessels, reduced postoperative pain and swelling (thus reducing the need for postoperative analgesics/narcotics), reduced bacterial counts, and a minimized need for sutures in most surgical procedures.
4. Although clinicians can control some of the factors that affect laser/tissue interactions, two factors remain independent of the operator: the unique characteristics of the laser wavelength’s emissions and the qualities inherent within the specific target tissue. Among the factors that clinicians can control are the power setting of the laser (power density), the total power delivered over a given surface area (energy density or fluence), the rate and duration of exposure (continuous versus pulsed, and pulse duration and repetition), and the method by which energy is delivered to the target tissue (contact versus non-contact)[2].
References:
[1]Steven, Mark, Eugenia, et al. Current Concepts of Laser–Oral Tissue Interaction[J]. Special Issue "Lasers in Dentistry: Hard and Soft Tissues" of Dentistry Journal, 2020.
[2]Lomke Mitchell A. Clinical Applications of Dental Lasers[J]. General Dentistry, 2015.