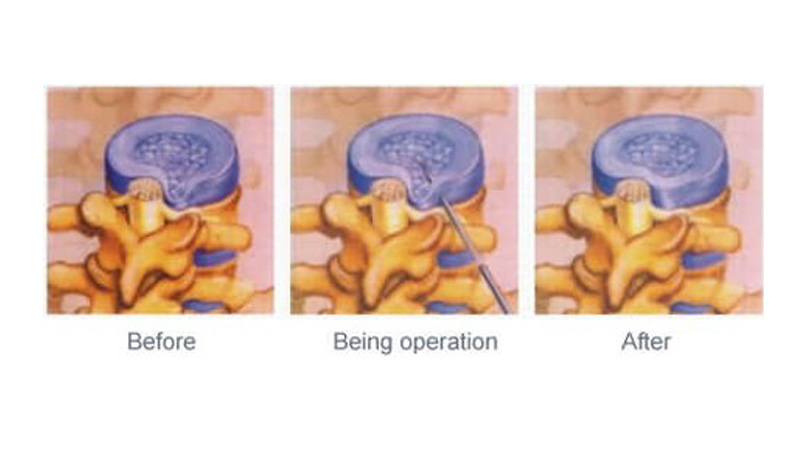
Percutaneous laser disc decompression (PLDD) is a procedure in which a surgical fiber probe is inserted into the disc space and the laser energy emitted by the fiber is applied to vaporize and ablate the nucleus pulposus to achieve decompression and neuromodulation and thus pain relief. It is a minimally invasive surgery with significant clinical advantages and falls under the category of percutaneous intervertebral surgery.
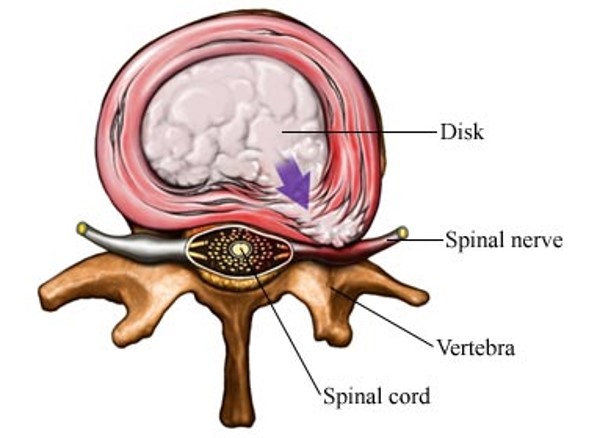
Understanding PLDD starts with understanding herniated discs. There are a total of 23 intervertebral discs distributed in the human spine, each consisting of a surrounding fibrous ring and a nucleus pulposus inside, like a balloon, which is very elastic. When the spine bends, the discs are compressed and share the pressure on the spine. As age grows and the spine becomes overstretched (engaged in physical labor), the elasticity of the discs decreases and difficult for them to contract automatically after being compressed, eventually forming a disc herniation and compressing the spinal nerves, causing pain in the spine and extremities. In this case, the process of ablating (vaporizing) part of the nucleus pulposus of the diseased disc by laser energy (usually 980nm laser), so that the contents of the individual disc become less and more easily contracted autonomously, is called PLDD.
A Step-by-Step Guide to Percutaneous Laser Disc Decompression (PLDD)
1.Preoperatively, the diseased disc is accurately determined by MRI imaging and analyzed for suitability for PLDD surgery.
2.Under local anesthesia, a skin puncture is performed at a suitable location in the lumbar region, and the fiber optic is aimed at the diseased disc under ultrasound guidance.
3.Introduction of laser energy into the nuclear pulposus percutaneously via a spinal needle and laser fiber.
4.Reduced the volume and pressure of a diseased disc without damaging other spinal structure.
5.After laser irradiation, intradisk pressure decrease and the nucleus pulposus is gradually replace by cartilage fibrous tissue.
6.Treatment completed, intracavity disinfection, skin surface disinfection.
Understanding the Core Components and Advantages of Percutaneous Laser Disc Decompression
1 Precise Localization
Ultrasound Imaging for Accurate Disc Localization
2 Controlled Laser Action
Point-like Controlled Energy for Minimized Tissue Damage
3 Minimal Side Effects
Achieving Short Recovery Time and Long-Term Non-Recurrence
At the heart of the Percutaneous Laser Disc Decompression (PLDD) procedure is the meticulous determination and localization facilitated by ultrasound imaging. This, coupled with the pinpoint accuracy of a surgical laser specially designed for PLDD, enables the entire process to unfold through a minimal skin incision, necessitating only local anesthesia.
The surgical laser's action is characterized by precision and control. When handled adeptly, it allows for optimal control over potential damage to surrounding tissues. This meticulous approach results in minimal side effects, a brief recovery period, and a reduced likelihood of recurrence over the long term.
The integration of advanced surgical laser technology into PLDD enhances the precision and effectiveness of the procedure. The synergy between ultrasound imaging and the focused energy of the surgical laser not only streamlines the process but also ensures a higher degree of accuracy, contributing to the overall success and patient outcomes in PLDD.